The latest global coronavirus stats are approaching half a million confirmed cases. At the frontlines in this endless fight against the spread of this disease are doctors and nurses.

One of these doctors, Nathalie Ververs, works in the Catharina Hospital’s emergency department. “And there she sees what the coronavirus can do to people. And she sees the numbers increasing,” reads a press statement released from the hospital.
Dr Ververs made a spontaneous plea on social media after a very troubling night in the Emergency Room. “It is someone’s mom or dad dying. [There is] so much sadness for so many people. I hope people will realise the virus does not spread itself. People do. People, please stay inside!”
Recovering patients say, ‘Do not underestimate this disease’
“I got really sick and could not sleep because of the headache. My muscles wasted away, and I was no longer hungry. I could not go to the toilet or take a shower. I was shocked that it could almost destroy me”, Peter-Paul Zwanikken (58), from Huizen, says.
Peter-Paul has now almost recovered, but it took nearly a month. He, and other recovered patients, warn people not to underestimate the virus. The coronavirus leads to severe symptoms in about 20% of patients.
The Longfonds, a National NGO, is preparing for a new group of patients due to the coronavirus. According to the organisation, it is already clear that some COVID-19 patients have been left with permanent lung damage. According to them, patients who need to be given artificial respiration in intensive care are at particular risk.
More people left with lung issues
“Inflammation can occur that cause scar tissue to form on the lungs”, pulmonologist, Dr Leon van den Toorn, chairman of the Dutch Association of Lung Diseases and Tuberculosis says. “This could mean there will soon be many more people with lung problems. It will be a new lung disease.”
Longfonds Director, Michael Rutgers, says it is essential that solutions are developed now for the future group of patients. Together with the Dutch Lung Alliance, the fund is developing a research programme. This will be done on this “new pulmonary disease”.
It has been named Corona Obstructive Lung Disease (COLD), for now. This will make it possible to map out the consequences of the coronavirus infection on lung function and on the patients’ lives after their recovery.
‘Lack of protective gear puts PGB holders at risk’
The scarcity of protective equipment, such as gloves and disinfectants, is also causing problems for other groups of people. Included are those in need of care with a personal budget (PGB). This was reported on KRO-NCRV’s radio’s Reporter. People with a PGB have to pay for their own care. However, according to an advocate for 130,000 PGB people “get pushed to the back of the queue”.
Some of these people have to be ventilated at home or need protection equipment for another reason. “Because of the coronavirus, this equipment is scarce. That is causing concern among our clients”, Aline Molenaar, from the watchdog, Per Saldo, said during the programme.
“You are dealing with people who are very susceptible to all kinds of viruses and infections”. At EMB Nederland – an interest group for parents with children with multiple disabilities – they have also seen a shortage of protective equipment. Caregivers are not always protected. This poses a considerable risk to children who, for example, suffer from lung and muscle diseases.
Blood bank wants to collect plasma from recovered patients
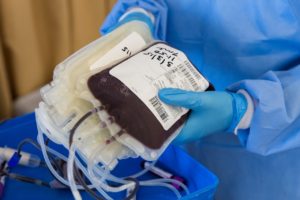
Sanquin’s blood banks have started collecting blood plasma from patients who have recovered from this virus. Hospitals are looking at whether antibodies present in the plasma of recovered coronavirus patients help to reduce corona symptoms in other patients.
This could, for example, prevent a patient from ending up in intensive care. It is not a standard treatment, Sanquin emphasises. It is a study of the effectiveness of blood plasma as a treatment protocol. People who have had COVID-19 have received an invitation via the Municipal Health Service (GGD) to report to Sanquin.
They are asked to donate plasma a total of four times, at seven-day intervals. “This is safe and not very stressful for the recovered patients”, a spokesperson from the blood bank promises. People suffering from the coronavirus can then be transfused. They will receive antibodies Sanquin has extracted from the plasma.
Doctors can then see whether this treatment can help combat the virus and help reduce patients’ physical reaction to the disease.
Why are relatively few people dying in Germany?
The number of coronavirus infections is increasing rapidly worldwide. In Germany, the virus has been detected in more than 35,700 people. It is, however, striking that there are relatively few deaths there – 181 so far.
How is that possible? Several experts have looked into this. They have not come up with a single identifiable cause but mention a few factors that could have a potential influence. The most common explanation is that Germany did wide-spread testing from early on. That means many patients with mild symptoms have been identified and, therefore, included in the statistics.
The German figures are, therefore, be a more realistic reflection of the number of sick people in that country. In other countries, the number of ill people not known to the authorities is expected to be much higher. According to a spokesman of the Robert Koch Institut (RKI), the German RIVM, German authorities were alarmed about the virus at an early stage.
“At the end of January, we already had a small coronavirus outbreak in Bavaria, at a company called Webasto. We managed to isolate it well, but from that moment on, we took it seriously. That is why we immediately started testing a lot of people. We also quarantined people from, for example, high-risk areas in China for two weeks.”
160,000 tests a week
According to the German Health Minister Jens Spahn, the test capacity in that country is 200,000 per week. Some 160,000 tests have been carried out per week. In the Netherlands, according to RIVM figures, slightly less than 20,000 tests were carried out this week. That totals between 1,900 and 3,500 per day.
German doctors are allowed to decide for themselves who they want to test. The RKI’s guideline is strict, albeit slightly less stringent than in the Netherlands. In the Netherlands, tests are only carried out on very sick people. The RKI, however, tests on people who have coronavirus-like symptoms and were in a high-risk area or were in contact with an infected person.
The average age of the patients in Germany is still relatively low, namely 45. In Italy, it is 63. It is well known that the older the patient is, the higher the chance that he or she will die from this disease. So it is logical that if the group of patients is, on average, younger, the number of deaths will be lower.
Because of this low average age, experts warn against premature conclusions. According to virologist, Alexander Kékulé, it may well be that the death toll will increase considerably in the coming weeks. These young people may well have infected older people too.
Pandemic still in its infancy
“We are still at the beginning of this pandemic. People are sick, but that battle sometimes lasts for weeks. First comes the wave of the sick, then comes the wave of the dead. In Italy, they did not get that first wave of sick people at all. They realised far too late what was going on”, Kékulé says in his daily podcast.
At the moment the hospitals in Germany are not overloaded either. Germany has the highest number of ICU beds in Europe – 28,000. Of these, 25,000 are equipped with respirators.
All coronary patients in that country are currently still receiving optimal treatment. According to Kékulé, this too could change in the coming weeks: “If we get more people who are seriously ill, things could become tighter for us as well.”
Sources: Catharina Hospital, NOS, the Longfonds
Translators: Bob and Melinda Walraven
Editor: Melinda Walraven










